Extragonadal Germ Cell Tumors Treatment (PDQ®): Treatment – Patient Information [NCI]
This information is produced and provided by the National Cancer Institute (NCI). The information in this topic may have changed since it was written. For the most current information, contact the National Cancer Institute via the Internet web site at http://cancer.gov or call 1-800-4-CANCER.
General Information About Extragonadal Germ Cell Tumors
Extragonadal germ cell tumors form from developing sperm or egg cells that travel from the gonads to other parts of the body.
“Extragonadal” means outside of the gonads (sex organs). When cells that are meant to form sperm in the testicles or eggs in the ovaries travel to other parts of the body, they may grow into extragonadal germ cell tumors. These tumors may begin to grow anywhere in the body but usually begin in organs such as the pineal gland in the brain, in the mediastinum (area between the lungs), or in the retroperitoneum (the back wall of the abdomen).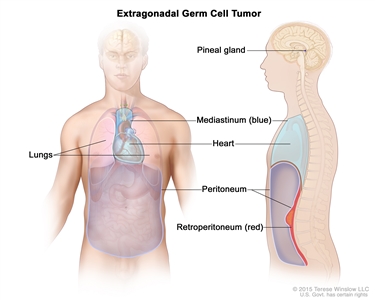
Extragonadal germ cell tumors form in parts of the body other than the gonads (testicles or ovaries). This includes the pineal gland in the brain, the mediastinum (area between the lungs), and retroperitoneum (the back wall of the abdomen).
Extragonadal germ cell tumors can be benign (noncancer) or malignant (cancer). Benign extragonadal germ cell tumors are called benign teratomas. These are more common than malignant extragonadal germ cell tumors and often are very large.
Malignant extragonadal germ cell tumors are divided into two types, nonseminoma and seminoma. Nonseminomas tend to grow and spread more quickly than seminomas. They usually are large and cause signs and symptoms. If untreated, malignant extragonadal germ cell tumors may spread to the lungs, lymph nodes, bones, liver, or other parts of the body.
For information about germ cell tumors in the ovaries and testicles, see the following PDQ summaries:
- Ovarian Germ Cell Tumors Treatment
- Testicular Cancer Treatment
Age and gender can affect the risk of extragonadal germ cell tumors.
Anything that increases your chance of getting a disease is called a risk factor. Having a risk factor does not mean that you will get cancer; not having risk factors doesn’t mean that you will not get cancer. Talk with your doctor if you think you may be at risk. Risk factors for malignant extragonadal germ cell tumors include the following:
- Being male.
- Being age 20 or older.
- Having Klinefelter syndrome.
Signs and symptoms of extragonadal germ cell tumors include breathing problems and chest pain.
Malignant extragonadal germ cell tumors may cause signs and symptoms as they grow into nearby areas. Other conditions may cause the same signs and symptoms. Check with your doctor if you have any of the following:
- Chest pain.
- Breathing problems.
- Cough.
- Fever.
- Headache.
- Change in bowel habits.
- Feeling very tired.
- Trouble walking.
- Trouble in seeing or moving the eyes.
Imaging and blood tests are used to detect (find) and diagnose extragonadal germ cell tumors.
The following tests and procedures may be used:
- Physical exam and history: An exam of the body to check general signs of health, including checking for signs of disease, such as lumps or anything else that seems unusual. The testicles may be checked for lumps, swelling, or pain. A history of the patient’s health habits and past illnesses and treatments will also be taken.
- Chest x-ray: An x-ray of the organs and bones inside the chest. An x-ray is a type of energy beam that can go through the body and onto film, making a picture of areas inside the body.
- Serum tumor marker test: A procedure in which a sample of blood is examined to measure the amounts of certain substances released into the blood by organs, tissues, or tumor cells in the body. Certain substances are linked to specific types of cancer when found in increased levels in the blood. These are called tumor markers. The following three tumor markers are used to detect extragonadal germ cell tumor:
- Alpha-fetoprotein (AFP).
- Beta-human chorionic gonadotropin (β-hCG).
- Lactate dehydrogenase (LDH).
Blood levels of the tumor markers help determine if the tumor is a seminoma or nonseminoma.
- CT scan (CAT scan): A procedure that makes a series of detailed pictures of areas inside the body, taken from different angles. The pictures are made by a computer linked to an x-ray machine. A dye may be injected into a vein or swallowed to help the organs or tissues show up more clearly. This procedure is also called computed tomography, computerized tomography, or computerized axial tomography.
Sometimes a CT scan and a PET scan are done at the same time. A PET scan is a procedure to find malignant tumor cells in the body. A small amount of radioactive glucose (sugar) is injected into a vein. The PET scanner rotates around the body and makes a picture of where glucose is being used in the body. Malignant tumor cells show up brighter in the picture because they are more active and take up more glucose than normal cells do. When a PET scan and CT scan are done at the same time, it is called a PET-CT.
- Biopsy: The removal of cells or tissues so they can be viewed under a microscope by a pathologist to check for signs of cancer. The type of biopsy used depends on where the extragonadal germ cell tumor is found.
- Excisional biopsy: The removal of an entire lump of tissue.
- Incisional biopsy: The removal of part of a lump or sample of tissue.
- Core biopsy: The removal of tissue using a wide needle.
- Fine-needle aspiration (FNA) biopsy: The removal of tissue or fluid using a thin needle.
Certain factors affect prognosis (chance of recovery) and treatment options.
The prognosis (chance of recovery) and treatment options depend on the following:
- Whether the tumor is nonseminoma or seminoma.
- The size of the tumor and where it is in the body.
- The blood levels of AFP, β-hCG, and LDH.
- Whether the tumor has spread to other parts of the body.
- The way the tumor responds to initial treatment.
- Whether the tumor has just been diagnosed or has recurred (come back).
Stages of Extragonadal Germ Cell Tumors
After an extragonadal germ cell tumor has been diagnosed, tests are done to find out if cancer cells have spread to other parts of the body.
The extent or spread of cancer is usually described as stages. For extragonadal germ cell tumors, prognostic groups are used instead of stages. The tumors are grouped according to how well the cancer is expected to respond to treatment. It is important to know the prognostic group in order to plan treatment.
There are three ways that cancer spreads in the body.
Cancer can spread through tissue, the lymph system, and the blood:
- Tissue. The cancer spreads from where it began by growing into nearby areas.
- Lymph system. The cancer spreads from where it began by getting into the lymph system. The cancer travels through the lymph vessels to other parts of the body.
- Blood. The cancer spreads from where it began by getting into the blood. The cancer travels through the blood vessels to other parts of the body.
Cancer may spread from where it began to other parts of the body.
When cancer spreads to another part of the body, it is called metastasis. Cancer cells break away from where they began (the primary tumor) and travel through the lymph system or blood.
- Lymph system. The cancer gets into the lymph system, travels through the lymph vessels, and forms a tumor (metastatic tumor) in another part of the body.
- Blood. The cancer gets into the blood, travels through the blood vessels, and forms a tumor (metastatic tumor) in another part of the body.
The metastatic tumor is the same type of tumor as the primary tumor. For example, if an extragonadal germ cell tumor spreads to the lung, the tumor cells in the lung are actually cancerous germ cells. The disease is metastatic extragonadal germ cell tumor, not lung cancer.
The following prognostic groups are used for extragonadal germ cell tumors:
Good prognosis
A nonseminoma extragonadal germ cell tumor is in the good prognosis group if:
- the tumor is in the back of the abdomen; and
- the tumor has not spread to organs other than the lungs; and
- the levels of tumor markers AFP and β-hCG are normal and LDH is slightly above normal.
A seminoma extragonadal germ cell tumor is in the good prognosis group if:
- the tumor has not spread to organs other than the lungs; and
- the level of AFP is normal; β-hCG and LDH may be at any level.
Intermediate prognosis
A nonseminoma extragonadal germ cell tumor is in the intermediate prognosis group if:
- the tumor is in the back of the abdomen; and
- the tumor has not spread to organs other than the lungs; and
- the level of any one of the tumor markers (AFP, β-hCG, or LDH) is more than slightly above normal.
A seminoma extragonadal germ cell tumor is in the intermediate prognosis group if:
- the tumor has spread to organs other than the lungs; and
- the level of AFP is normal; β-hCG and LDH may be at any level.
Poor prognosis
A nonseminoma extragonadal germ cell tumor is in the poor prognosis group if:
- the tumor is in the chest; or
- the tumor has spread to organs other than the lungs; or
- the level of any one of the tumor markers (AFP, β-hCG, or LDH) is high.
Seminoma extragonadal germ cell tumor does not have a poor prognosis group.
Treatment Option Overview
There are different types of treatment for patients with extragonadal germ cell tumors.
Different types of treatments are available for patients with extragonadal germ cell tumors. Some treatments are standard (the currently used treatment), and some are being tested in clinical trials. A treatment clinical trial is a research study meant to help improve current treatments or obtain information on new treatments for patients with cancer. When clinical trials show that a new treatment is better than the standard treatment, the new treatment may become the standard treatment. Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Three types of standard treatment are used:
Radiation therapy
Radiation therapy is a cancer treatment that uses high-energy x-rays or other types of radiation to kill cancer cells or keep them from growing. There are two types of radiation therapy:
- External radiation therapy uses a machine outside the body to send radiation toward the cancer.
- Internal radiation therapy uses a radioactive substance sealed in needles, seeds, wires, or catheters that are placed directly into or near the cancer.
The way the radiation therapy is given depends on the type and stage of the cancer being treated. External radiation therapy is used to treat seminoma.
Chemotherapy
Chemotherapy is a cancer treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. When chemotherapy is taken by mouth or injected into a vein or muscle, the drugs enter the bloodstream and can reach cancer cells throughout the body (systemic chemotherapy). When chemotherapy is placed directly in the cerebrospinal fluid, an organ, or a body cavity such as the abdomen, the drugs mainly affect cancer cells in those areas (regional chemotherapy). The way the chemotherapy is given depends on the type and stage of the cancer being treated.
Surgery
Patients who have benign tumors or tumor remaining after chemotherapy or radiation therapy may need to have surgery.
New types of treatment are being tested in clinical trials.
This summary section describes treatments that are being studied in clinical trials. It may not mention every new treatment being studied. Information about clinical trials is available from the NCI website.
High-dose chemotherapy with stem cell transplant
High doses of chemotherapy are given to kill cancer cells. Healthy cells, including blood-forming cells, are also destroyed by the cancer treatment. Stem cell transplant is a treatment to replace the blood -forming cells. Stem cells (immature blood cells) are removed from the blood or bone marrow of the patient or a donor and are frozen and stored. After the patient completes chemotherapy, the stored stem cells are thawed and given back to the patient through an infusion. These reinfused stem cells grow into (and restore) the body’s blood cells.
Treatment for extragonadal germ cell tumors may cause side effects.
For information about side effects caused by treatment for cancer, see our Side Effects page.
Patients may want to think about taking part in a clinical trial.
For some patients, taking part in a clinical trial may be the best treatment choice. Clinical trials are part of the cancer research process. Clinical trials are done to find out if new cancer treatments are safe and effective or better than the standard treatment.
Many of today’s standard treatments for cancer are based on earlier clinical trials. Patients who take part in a clinical trial may receive the standard treatment or be among the first to receive a new treatment.
Patients who take part in clinical trials also help improve the way cancer will be treated in the future. Even when clinical trials do not lead to effective new treatments, they often answer important questions and help move research forward.
Patients can enter clinical trials before, during, or after starting their cancer treatment.
Some clinical trials only include patients who have not yet received treatment. Other trials test treatments for patients whose cancer has not gotten better. There are also clinical trials that test new ways to stop cancer from recurring (coming back) or reduce the side effects of cancer treatment.
Clinical trials are taking place in many parts of the country. Information about clinical trials supported by NCI can be found on NCI’s clinical trials search webpage. Clinical trials supported by other organizations can be found on the ClinicalTrials.gov website.
Follow-up tests may be needed.
Some of the tests that were done to diagnose the cancer or to find out the stage of the cancer may be repeated. Some tests will be repeated in order to see how well the treatment is working. Decisions about whether to continue, change, or stop treatment may be based on the results of these tests.
Some of the tests will continue to be done from time to time after treatment has ended. The results of these tests can show if your condition has changed or if the cancer has recurred (come back). These tests are sometimes called follow-up tests or check-ups.
After initial treatment for extragonadal germ cell tumors, blood levels of AFP and other tumor markers continue to be checked to find out how well the treatment is working.
Treatment Options for Extragonadal Germ Cell Tumors
For information about the treatments listed below, see the Treatment Option Overview section.
Benign Teratoma
Treatment of benign teratomas is surgery.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Seminoma
Treatment of seminoma extragonadal germ cell tumors may include the following:
- Radiation therapy for small tumors in one area, followed by watchful waiting if there is tumor remaining after treatment.
- Chemotherapy for larger tumors or tumors that have spread. If a tumor smaller than 3 centimeters remains after chemotherapy, watchful waiting follows. If a larger tumor remains after treatment, surgery or watchful waiting follow.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Nonseminoma
Treatment of nonseminoma extragonadal germ cell tumors may include the following:
- Combination chemotherapy followed by surgery to remove any remaining tumor.
- A clinical trial of a new treatment.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
Recurrent or Refractory Extragonadal Germ Cell Tumors
Treatment of extragonadal germ cell tumors that are recurrent (come back after being treated) or refractory (do not get better during treatment) may include the following:
- Chemotherapy.
- A clinical trial of high-dose chemotherapy with stem cell transplant.
- A clinical trial of a new treatment.
Use our clinical trial search to find NCI-supported cancer clinical trials that are accepting patients. You can search for trials based on the type of cancer, the age of the patient, and where the trials are being done. General information about clinical trials is also available.
To Learn More About Extragonadal Germ Cell Tumors
For more information from the National Cancer Institute about extragonadal germ cell tumors, see the Extragonadal Germ Cell Tumor Home Page.
For general cancer information and other resources from the National Cancer Institute, see the following:
- About Cancer
- Staging
- Chemotherapy and You: Support for People With Cancer
- Radiation Therapy and You: Support for People With Cancer
- Coping with Cancer
- Questions to Ask Your Doctor about Cancer
- For Survivors and Caregivers
About This PDQ Summary
About PDQ
Physician Data Query (PDQ) is the National Cancer Institute’s (NCI’s) comprehensive cancer information database. The PDQ database contains summaries of the latest published information on cancer prevention, detection, genetics, treatment, supportive care, and complementary and alternative medicine. Most summaries come in two versions. The health professional versions have detailed information written in technical language. The patient versions are written in easy-to-understand, nontechnical language. Both versions have cancer information that is accurate and up to date and most versions are also available in Spanish.
PDQ is a service of the NCI. The NCI is part of the National Institutes of Health (NIH). NIH is the federal government’s center of biomedical research. The PDQ summaries are based on an independent review of the medical literature. They are not policy statements of the NCI or the NIH.
Purpose of This Summary
This PDQ cancer information summary has current information about the treatment of extragonadal germ cell tumors. It is meant to inform and help patients, families, and caregivers. It does not give formal guidelines or recommendations for making decisions about health care.
Reviewers and Updates
Editorial Boards write the PDQ cancer information summaries and keep them up to date. These Boards are made up of experts in cancer treatment and other specialties related to cancer. The summaries are reviewed regularly and changes are made when there is new information. The date on each summary (“Updated”) is the date of the most recent change.
The information in this patient summary was taken from the health professional version, which is reviewed regularly and updated as needed, by the PDQ Adult Treatment Editorial Board.
Clinical Trial Information
A clinical trial is a study to answer a scientific question, such as whether one treatment is better than another. Trials are based on past studies and what has been learned in the laboratory. Each trial answers certain scientific questions in order to find new and better ways to help cancer patients. During treatment clinical trials, information is collected about the effects of a new treatment and how well it works. If a clinical trial shows that a new treatment is better than one currently being used, the new treatment may become “standard.” Patients may want to think about taking part in a clinical trial. Some clinical trials are open only to patients who have not started treatment.
Clinical trials can be found online at NCI’s website. For more information, call the Cancer Information Service (CIS), NCI’s contact center, at 1-800-4-CANCER (1-800-422-6237).
Permission to Use This Summary
PDQ is a registered trademark. The content of PDQ documents can be used freely as text. It cannot be identified as an NCI PDQ cancer information summary unless the whole summary is shown and it is updated regularly. However, a user would be allowed to write a sentence such as “NCI’s PDQ cancer information summary about breast cancer prevention states the risks in the following way: [include excerpt from the summary].”
The best way to cite this PDQ summary is:
PDQ® Adult Treatment Editorial Board. PDQ Extragonadal Germ Cell Tumors Treatment. Bethesda, MD: National Cancer Institute. Updated <MM/DD/YYYY>. Available at: https://www.cancer.gov/types/extragonadal-germ-cell/patient/extragonadal-treatment-pdq. Accessed <MM/DD/YYYY>. [PMID: 26389213]
Images in this summary are used with permission of the author(s), artist, and/or publisher for use in the PDQ summaries only. If you want to use an image from a PDQ summary and you are not using the whole summary, you must get permission from the owner. It cannot be given by the National Cancer Institute. Information about using the images in this summary, along with many other images related to cancer can be found in Visuals Online. Visuals Online is a collection of more than 3,000 scientific images.
Disclaimer
The information in these summaries should not be used to make decisions about insurance reimbursement. More information on insurance coverage is available on Cancer.gov on the Managing Cancer Care page.
Contact Us
More information about contacting us or receiving help with the Cancer.gov website can be found on our Contact Us for Help page. Questions can also be submitted to Cancer.gov through the website’s E-mail Us.
Last Revised: 2019-03-07
If you want to know more about cancer and how it is treated, or if you wish to know about clinical trials for your type of cancer, you can call the NCI’s Cancer Information Service at 1-800-422-6237, toll free. A trained information specialist can talk with you and answer your questions.
This information does not replace the advice of a doctor. Healthwise, Incorporated, disclaims any warranty or liability for your use of this information. Your use of this information means that you agree to the Terms of Use. Learn how we develop our content.

